The Lancaster Health and Medical Museum Collection, an affiliated society of BSHM, publishes a short article each month about one of the treasured objects in their collection. Bryan Rhodes describes how one of these objects revealed a hidden book by a remarkable author.
This week marks International Nurses’ Day, and this blog celebrates an interesting nurse dictionary donated to our collection some years ago by an elderly nurse who had trained in Lancaster. Having chosen to feature this book, A New Dictionary for Nurses by Lois Oakes, as our ‘Object of the Month’ for March 2026 on the Lancaster Health and Medical Museum website, I discovered a completely different nurse dictionary hidden inside its damaged cover.
The hidden book’s remarkable author was Violet Honnor Morten (1861 – 1913), who preferred to be known as Honnor Morten. Honnor Morten was not just a nurse and a writer, but also a social activist who lectured widely on family health, women’s rights and nursing care.
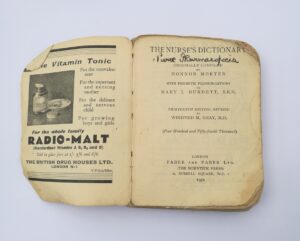
A New Dictionary for Nurses by Lois Oakes is small (12 x 9 cm /4.5 x 3.5 inches) and was clearly designed to fit into a pocket. Its well-thumbed and taped cover indicates how much the book was used over the years. The front cover shows that it was first published in 1932. This book, which subsequently became the ‘Churchill Livingstone’s Dictionary of Nursing’, was last published in 2006, the 19th edition.
However, the bulk of the contents, easily separated from the cover, is from another pocket-sized nurse dictionary: The Nurse’s Dictionary by Honner Morten, 13th edition, also published in 1932 by Faber and Faber. In 246 pages, featuring entries from abdomen to zymotic, appears to be a complete Honnor Morten dictionary,
The small photograph found inside the book has the inscription ‘Alder Hey 1932-35’ on the reverse, and the date 1932 is also hand-written inside the red cover.
Honner Morten’s dictionary is almost certainly the most successful nursing publication of all time, achieving 30 editions until the 1980s by Faber and Faber, with three further editions published by Mosby. The final 33rd, edition, entitled Mosby Nurse’s Pocket Dictionary, came out in 2005.
Who was Honnor Morten?
(Violet) Honnor Morten (1861-1913), nurse, author and activist, was born in Surrey and was the daughter of a wealthy solicitor and the niece of a successful author called William Black. She started her nurse training in 1881 at the London Hospital and then studied midwifery before gaining a diploma in scientific hygiene at Bedford College, London. A prolific writer, she contributed articles to The Hospital journal, and the same publisher, Scientific Press, published the first edition of her dictionary in 1891. Then titled Nurse’s Dictionary of Medical Terms and Nursing Treatment, it was the first such dictionary dedicated to nurses. The book went through eight editions in her lifetime and was very successful. This book became The Nurse’s Dictionary, ultimately achieving 33 editions. She also wrote a number of other books between 1888 and 1912, mostly on subjects related to nursing, midwifery or childcare.
An avowed socialist and non-militant suffragist, Morten lectured widely on family health, women’s rights and nursing care. During the campaign for women’s voting rights, she joined others in refusing to pay taxes, resulting in the confiscation and auctioning of some of her property. She was a founder member of a number of societies including the Women’s Writers Club, the Association of Asylum Workers, the Nurse’s Co-operation and the School Nurses’ Society. The latter was involved in efforts to provide countryside respite care for disabled children, and Morten supported this aim by establishing a centre in Rotherfield, Sussex in 1905 for disabled children from London.
A keen smoker at a time when the health risks of smoking were not understood, she died of throat cancer the year before the first world war began, aged just 52. Her most abiding legacy is the pioneering nurse dictionary which continued to inform nurse trainees more than a century after its first publication.
Bryan Rhodes is the chair of the Lancaster Health and Medical Museum Collection. He is a retired orthopaedic surgeon. He is vice-president of the British Society for the History of Medicine and was guest editor of the 5th edition of the BSHM journal Topics in the History of Medicine.
Further reading:
Ross, E. (2022, May 12). Morten, (Violet) Honnor (1861–1913), nurse and journalist. Oxford Dictionary of National Biography. Retrieved 15 Apr. 2026